Following diagnosis of stomach (gastric) or oesophageal (gullet) cancer
Your consultant will have explained to you that you have a cancer of the Upper Gastro-Intestinal tract (Upper GI) affecting either your stomach or oesophagus (gullet). Being told you have cancer is naturally a shock to you and your family. During this time, you may experience a wide range of emotions and find it difficult to remember all you are told. This information is provided as a guide to what may happen; however, your consultant will discuss your individual treatment plan with you. Included is information about investigations you may have, treatments or procedures that may be recommended and what to expect next. Contact information for individuals who may be involved in your care are also included at the end of this page.
This information is provided as a guide to what may happen; however, your consultant will discuss your individual treatment plan with you.
Included is information about investigations you may have, treatments or procedures that may be recommended and what to expect next. Contact information for individuals who may be involved in your care are also included at the end of this page.
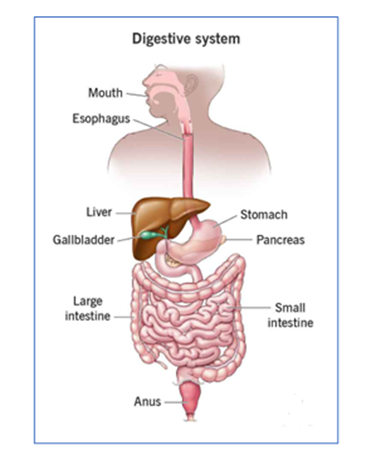
Investigations
Various investigations may be required to assess the extent (stage) of your cancer and your fitness levels to help plan the appropriate treatment for you. Details of the common investigations can be found on the following pages.
To assess the cancer
Endoscopy
A flexible tube with a camera is passed through the mouth, down the oesophagus into the stomach. Before this happens, a throat spray (local anaesthetic) is used to numb the back of the throat and sometimes sedation can also be given. Please note that you will need someone to take you home and stay with you that evening if you have sedation.
If there are any abnormal areas seen during the procedure, the doctor will take a biopsy (tissue sample). The biopsy will be sent to the laboratory for examination and the results can take 1 to 2 weeks to come through. Occasionally, the endoscopy and biopsies need to be repeated.
CT Scan (Computerised Tomography)
A detailed scan of your chest, abdomen and pelvis will be performed in our Imaging (X-ray) Department. You may be asked to drink some dye (contrast) before the procedure and also have an injection of dye while lying on the X-ray bed. The dye is used to enhance the scan images.
PET Scan (Positron Emission Tomography)
This is another type of scan used to assess the extent (stage) of cancer. A radioactive sugary substance is given to you via an injection. This substance is taken up by the area(s) of cancer and will highlight cancer activity on the scan images.
You will need to travel to the Cobalt Imaging Centre in Cheltenham to have this done.
Abdominal laparoscopy (can also be referred as staging laparoscopy)
A short keyhole operation performed in theatre under general anaesthetic (GA), while you are asleep. This involves a couple of small incisions being made in the abdomen so that a thin instrument with a camera can be passed inside the abdomen to examine the area of cancer and nearby structures. Occasionally, further biopsies are taken during this procedure. The abdominal laparoscopy is usually done as a day case procedure but sometimes it may involve an overnight stay. You may feel sore for a couple of days following this procedure.
EUS ( Endoscopic Ultrasound Scan)
This is similar to the endoscopy you have already had, however, the endoscope has an ultrasound probe attached to it. This allows an internal scan of your oesophagus to be performed, which can also assess the surrounding lymph nodes (glands).
Blood tests
You may need bloods tests to measure the level of nutrients in the blood that are needed to produce red blood cells. If your blood levels are low then you may need to have supplements. This may be tablets, injections or an iron infusion.
If you are being considered for chemotherapy you may also have an additional blood test to help plan chemotherapy treatment.
To assess your fitness
ECHO (Echocardiogram)
This is an ultrasound scan of the heart which gives information about how well your heart is working. It will look at the structure of your heart, how the blood flows and assess the pumping chambers of the heart.
Pulmonary Function Test (PFT)
A test of the lungs which gives information about how well your lungs are working. A spirometer is used to measure how much air you can breathe out in one forced breath.
Anaesthetic assessment
If an operation is thought to be suitable to remove your cancer you will have an anaesthetic assessment. This is an appointment with a nurse and an anaesthetist. They will ask you questions about your health, other medical problems, medications and fitness. They will perform blood tests and record an electrocardiogram (ECG) and look at the results of your heart and lung tests.
These results will inform them if surgery is suitable for you, or if you have any medical problems that may need to be treated before an operation.
Multidisciplinary team (MDT)
Following your investigations, the results will be discussed at the multi-disciplinary team meeting (MDT) which takes place every Thursday. This meeting is attended by surgeons, oncologists, physicians, pathologists, radiologists, nurse specialists, dietitians, and palliative care. The team will review your results and make a management plan on how to best treat/support your individual needs.
Occasionally, further investigations will be required such as, MRI scans, an ultrasound scan, a bone scan or further biopsies.
You will be updated about the outcome of this meeting either face to face in an out-patient clinic, by letter or by telephone.
Treatments and procedures
The treatment/procedure recommended for you will depend on the location, size, type of cancer, whether it has spread to other parts of the body (secondary cancer/metastases) and also your general level of fitness. Your treatment may involve one or a combination of the following:
Oncology treatments
If you are suitable to be considered for oncology treatment you will be referred to a specialist oncologist who will meet you in an out-patient clinic.
Following an assessment and discussion with you, they will inform you about the possible treatment options.
You will be given written information about the treatment planned.
If it is agreed you are having chemotherapy or immunotherapy an appointment will be made for you to meet the chemotherapy nurses who will give you additional information before starting treatment. The chemotherapy nurses will also be able to answer any questions you may have.
You will be reviewed regularly, by your oncologist, throughout your treatment and have access to a 24-hour telephone helpline (the telephone number can be found at the end of this page).
Chemotherapy
This is the use of anti-cancer (cytotoxic) drugs to destroy cancer cells. It may be used before surgery (neoadjuvant) to reduce the size of the cancer, after surgery (adjuvant) to reduce the risks of your cancer coming back or when surgery is not appropriate. Chemotherapy is usually given during an out-patient appointment, allowing you to go home the same day, although occasionally you may need to stay overnight. Chemotherapy is likely to be given into a vein (intravenously) and/or in tablet form.
Immunotherapy
Immunotherapy is the use of medicines to help your own immune system find and attack cancer cells more effectively. Some tests may be needed using your previous biopsy samples to see if this is suitable for you.
You may have immunotherapy on its own or alongside other chemotherapy treatments. Immunotherapy may also be recommended for some people following an operation to remove their cancer.
Targeted therapy
Sometimes targeted therapy with a drug called Trastuzumab is given. The drug can attach to proteins on the surface of cancer cells to try to stop the cancer growing. This can be given alongside chemotherapy and on its own after chemotherapy has finished.
Your previous biopsy samples would be tested to see if this is suitable for you.
Radiotherapy
The use of high energy rays to destroy cancer cells directed at specific areas of your body while doing as little harm as possible to normal cells. Radiotherapy can be given to shrink the tumour, improve symptoms and reduce or stop bleeding related to stomach cancers.
You will need a radiotherapy planning CT scan before starting your treatment. During the CT scan, tiny marks (tattoos) will be placed on your skin to mark where the treatment needs to be directed, this can be a little uncomfortable.
If the cancer is in the upper part of your oesophagus, a mask (shell) may be made for you to wear. This is to help make sure that the right area is treated.
Treatment usually runs on consecutive week days through the length of your treatment for the recommended duration, as discussed with the oncologist. Each treatment lasts approximately 10 to 15 minutes.
Surgery
If your investigations indicate that it is possible to remove your cancer with an operation and you are fit enough, then surgery will be discussed with you. The majority of patients will have chemotherapy or chemotherapy and radiotherapy before their surgery, unless the investigations you had indicate a very early-stage cancer. You may also need oncology treatment after the operation.
Upper GI surgery is a major operation that is likely to require you to be in hospital between 7 to 10 days, dependant on what type of surgery you are having. You will go to our Surgical High Dependency Unit following your operation with the aim to transfer to the ward when suitable.
You will be informed of our Enhanced Recovery After Surgery programme (ERAS). This is a programme aimed at reducing complications and to get you home earlier, fitter and safer. This will be discussed with you. You will also be given written information about your operation.
Oesophageal stent
A stent is a hollow tube that can be placed in the oesophagus if you have swallowing difficulties. This will allow foods and liquids to pass through. The stent is inserted in to the oesophagus endoscopically with X-ray guidance. This is usually done as a day case but sometimes requires an overnight stay in hospital. You will need an adult with you for the first night if you go home the same day as the procedure.
Dilatation
This is an endoscopic procedure, performed with a local anaesthetic throat spray and sedation, where the oesophagus can be stretched (dilated) to allow you to swallow more easily. This procedure is usually performed as a day case, though it is advised that you have an adult with you for the first night following the procedure.
Supportive care
The focus of supportive care is to improve your quality of life, addressing any issues you have with regard to symptoms, physical, psychological and social needs with the specialist input of community services.
You may be referred to our Enhanced Supportive Care team (ESC) or our Community Palliative Care team, depending on your needs.
Prehabilitation (prehab)
If it is planned for you to have treatment, you are likely to have side effects and feel tired from the treatment you receive. Surgery, as previously described, is a very big operation. To help you cope with any of the treatments you receive and aid your recovery there are some things you can do to help yourself. Your nurse specialist and dietitian will discuss this with you.
You may also be referred to our Prehab team. The Prehab team consists of a physiotherapist, dietitian and clinical psychologist. They will offer you a programme of support and advice to prepare and support you through your treatment, focusing on your nutrition, fitness and emotional wellbeing.
How you can help
If you are having treatment, you will be strongly encouraged to maintain or improve your fitness levels and nutrition to the best of your ability. This will help you cope with treatments and recovery from treatments.
If you smoke and are being considered for surgery, you will be advised to stop. This is to help reduce your risks of complications following your operation. You are unlikely to have your operation if you do not stop smoking.
If you need help with this, please speak to a member of the team looking after you.
Nutrition
Your cancer or treatment is likely to cause some changes to your appetite and eating habits. You may have swallowing difficulties, a loss of appetite, weight loss, nausea and taste changes.
It is important to keep yourself as strong as possible to help you cope with any treatments you may have. Your consultant, nurse specialist, dietitian or GP can give you advice.
Interventions as described on this page may be recommended to help with your swallowing but there are other options that may be suggested.
The use of medications to help with pain, nausea and acid reflux/indigestion can also be helpful. Nutrition supplemented drinks are also available on prescription from either your hospital team or GP if it is thought appropriate.
What happens next?
Throughout your investigations and treatment, you will have regular contact from the doctors managing your care or/and the nurse specialists and dietitians.
Following completion of your treatment, you will have regular follow up appointments with either your surgeon, oncologist, nurse specialist or community team or a combination of them.
If you have any concerns in between your appointments, you should contact your nurse specialist, dietitian, palliative care nurse or Oncology helpline (the telephone numbers can be found at the end of this page) or your own GP.
Contact information
Surgeon’s secretaries
Mr Dwerryhouse
Tel: 0300 422 6658
Mr Higgs
Tel: 0300 422 6658
Mr Hornby
Tel: 0300 422 6658
Miss Upchurch
Tel: 0300 422 5953
Oncologist’s secretaries
Dr Candish
Tel: 0300 422 4925
Dr Elyan
Tel: 0300 422 4032
Nurse Specialists
Kelly Weir
Lisa Quemby
Helen Skidmore
Natasha Brooke
Kerry Blissett
Tel: 0300 422 6222
Cancer Support Worker
Annabel Mander
Tel: 0300 422 5374
Dietician
Tel: 0300 422 5506
Supportive Care
Enhanced Supportive Care
Tel: 0300 422 3448
Community Palliative Care
Tel: 0300 422 5370
Chemotherapy 24 Hour Helpline
Tel: 0300 422 3444
Further information
Car Parking
Patients attending Cheltenham Oncology Unit for treatment are entitled to free parking for the duration of their treatment.
A parking permit will be given to you before starting your treatment.
Reduced parking fees or free parking in Gloucestershire Royal and Cheltenham General Hospitals are considered in individual cases where:
- The patient has been in hospital for 14 days or more.
- The patient has been in the Department of Critical Care for 3 days or more.
- After being in hospital for 3 days with a palliative (not curable) condition.
- Carers passport if attending hospital to support the needs of a patient.
- An out-patient with multiple appointments in 1 week.
Parking forms are available from the hospital ward. The completed form needs to be signed by the nurse in charge on the ward then taken to the parking shop. This is situated at:
Gloucestershire Royal Hospital
Ground floor of multi-storey car park
Open Monday to Friday 9:00am to 8:30pm and Saturday 9:00am to 12:30pm
The Parking shop is closed on Sundays.
Cheltenham General Hospital
Sandford Road
Open Monday to Sunday, 9:00am to 5:00pm
Prescription charges
You are entitled to free prescriptions if you have been diagnosed with cancer. A FP92A form needs to be completed which you can get from your nurse specialist, hospital pharmacy and some GP surgeries.
This form must be signed by a healthcare professional and sent to the address on the form. You should receive your exemption card within 2 weeks of receipt.
Benefit advice
Having a cancer diagnosis can be expensive through the loss of income and additional travelling cost etc. There are a range of benefits available for people with cancer and you are advised to contact a benefits adviser to see if you are eligible and for help with claims. This is a free and confidential service.
Please contact your Nurse specialist, the Cancer Support Worker or one of the Community services for support. They can refer you to the Macmillan Citizens Advice Benefits team to help you with this.
Community support services
There are a range of community support services available. Referrals can be made to support your day to day living for a range of issues, such as improving symptoms, emotional support, provision of equipment or aids and financial advice.
Please discuss your concerns with the team involved in your care or your GP so the appropriate referrals can be made.
Charlies Cancer Support and Therapy Centre
A walk-in centre which offers friendship, support, holistic therapies, activities and events. They offer a wide range of therapies which are free of charge for people (and family members) affected by cancer. They also offer a childrens’ service with an experienced youth support worker.
The main centre is in Gloucester with satellite centres in the Forest of Dean, Cheltenham, Cirencester and Newent.
Charlies Therapy Centre, Unit 2, Madleaze Road, Gloucester GL1 5SJ
Tel: 07786 547439
Website: www.charlies.org.uk
Email: charlies2014@yahoo.co.uk
Maggies
A walk-in centre which offers support, advice and information for anyone affected by cancer, all in a very peaceful, relaxed atmosphere. No appointment or referral needed. Refreshments are provided, free of charge. Supported by healthcare professionals, offering various services.
Situated close to Cheltenham Oncology Centre, The Lodge, Cheltenham General Hospital, College Baths Road, Cheltenham GL53 7QB
Tel: 01242 250611
Email: cheltenham@maggiescentres.org
Website: www.maggiescentres.org
Oesophageal Patients Association
Former patients helping new patients. The group aims to help new patients and families cope with the difficulties arising as a result of treatment, providing support and encouragement.
22 Vulcan House, Vulcan Road, Solihull, West Midlands
Helpline: 0121 704 9860
Monday to Friday, 9:00am to 7:00pm
E-mail: enquiries@opa.org.uk
Website: www.opa.org.uk
GUTSY Patient and Carers Support Group
This group is for patients who are planned to have or have had treatment with an aim to cure them of their oesophageal or stomach cancer. It takes place every 3 months and is supported and attended by members of your healthcare team.
Speak to your nurse specialist, support worker or dietitian for more information.
Macmillan Next Steps Cancer Rehabilitation
A local cancer rehabilitation service to support patients who have completed treatment. Offering free support to improve and maintain health and wellbeing. Supported by various health care professionals working with you through video consultations, phone calls, workshops and email support.
Please speak to your nurse specialist or support worker for more information or you can self-refer by telephone or email:
Tel: 0300 421 6586
Email: nextsteps@ghc.nhs.uk
Hospices
The word hospice conjures up many different thoughts. Modern hospice care is about helping people to live well throughout their illness and not about just supporting people at the end of life. The staff aim to meet the needs of the patients, their families and carers with the support and expertise of their multi-professional team, working in partnership with community care teams to support people at home, day centre facilities and some providing in-patient stay. There is a wide range of services to support physical, emotional, social and spiritual needs. Also available are a range of creative and complimentary therapies such as: reflexology, massage, acupuncture and aromatherapy.
Sue Ryder Hospice
Leckhampton Court, Church Road, Leckhampton, Cheltenham GL53 0QJ
Tel: 01242 230 199
Website: www.sueryder.org
Longfields Hospice
Burleigh Lane, Minchinhampton Gloucestershire GL5 2PQ
Tel: 01453 886 868
E-mail: info@cotswoldcare.org.uk
Website: www.cotswoldcare.org.uk
Great Oaks – Dean Forest Hospice
The Gorse, Coleford, Gloucestershire GL16 8QE
Tel: 01594 811 910
E-mail: clerical@great-oaks.org.uk
Website: www.great-oaks.org.uk
FOCUS Cancer Information and Support Centre
Within Cheltenham Oncology Centre
Open Monday to Friday, 10:00am to 5:00pm
Tel: 0300 422 4414
Macmillan Hub
Within the Atrium, Gloucestershire Royal Hospital
Open Monday to Friday, 9.00am to 4.00pm
Tel: 0300 422 8880
Email: ghn-tr.macmillanhub@nhs.net
Citizens Advice Bureau
Tel: 01452 527202
Website: www.adviceguide.org.uk
Macmillan Cancer Line
Freephone Tel: 0808 800 0000
Monday to Friday, 8:00am to 8:00pm
Website: www.macmillan.org.uk
Surgery images
The pictures on the following page provide an idea of how your digestive system may look after your operation.
Please remember that everyone is different, and not all operations are the same. Your doctor or specialist nurse will be able to help if you have any questions about your operation.
Surgery images
The images below provide an idea of how your digestive system may look after your operation. Please remember that everyone is different, and not all operations are the same.
Your doctor or nurse specialist will be able to help if you have any questions about your operation.
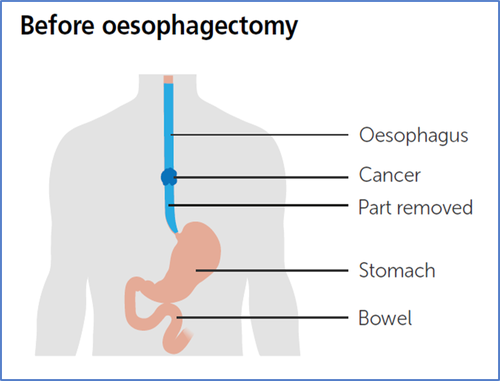
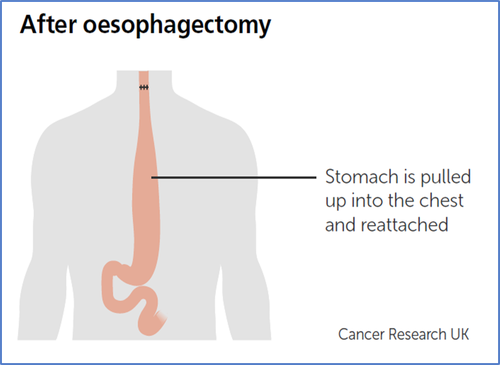
Oesophagectomy – involves removing part of your oesophagus (gullet and using the stomach to replace the tissue removed.
Total gastrectomy - in which the whole of the stomach in removed.
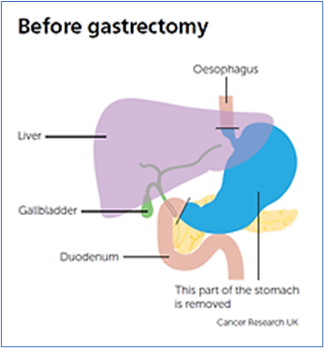
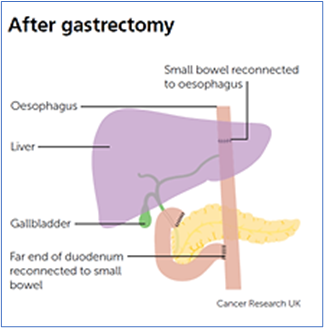
Partial gastrectomy - in which part of the stomach is removed.
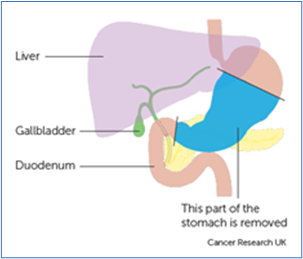
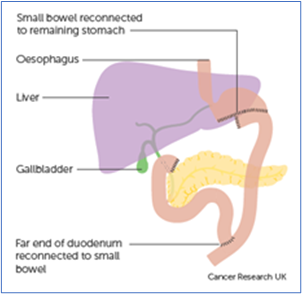
Images courtesy of Cancer Research UK