Having a ureteric stent
This page gives you information about having a ureteric stent placed in the ureter (the tube between your kidney and bladder). It also includes the benefits, risks and possible complications associated with a ureteric stent.
On this page
-
Why am I having a ureteric stent?
-
The urinary system and the ureter
-
How does a kidney become obstructed?
-
What are the effects of obstruction?
-
Temporary relief of the obstruction
-
What is a ureteric stent?
-
How does a stent stay in place?
-
Advantages of having a ureteric stent
-
How is a ureteric stent put in place?
-
How long will the stent stay in the body?
-
How is a stent removed?
-
Is there an alternative option?
-
Possible side effects
-
Commonly noted side effects
-
Can the side effects interfere with my day-to-day life?
-
Physical activities and sports
-
Work activities
-
Social life and interactions
-
Travel and holiday
-
Sex
-
What other complications are possible?
-
Is there a possibility of a urinary tract infection?
-
Self-care
-
When should I call for help?
-
Contact information
-
Further information
-
My Stent Details
Why am I having a ureteric stent?
A ureteric stent is used to prevent or temporarily relieve an obstruction (blockage) of the kidney.
The urinary system and the ureter
The kidneys produce urine. The urine produced in the kidney is carried to the bladder by a tube called the ureter. The bladder acts as a reservoir for the urine and when it is full it is emptied via the urethra (water pipe). See figure 1.
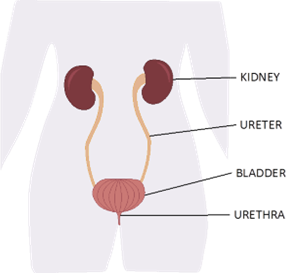
How does a kidney become obstructed?
Common causes of obstruction are:
- A kidney stone or stone fragment moving into the ureter, either spontaneously, or occasionally following treatment such as shock wave therapy.
- Narrowing (stricture) of the ureter. This can be due to scarring of the wall of the ureter, narrowing of the area where the ureter leaves the kidney (pelvi-ureteric junction) and compression from outside the wall of the ureter.
- Temporary tissue swelling or oedema of the ureter following an operation on or near the ureter and kidney.
- Diseases of the prostate or tumour of the urinary system.
Your urologist will discuss the cause of your obstruction with you in more detail.
What are the effects of obstruction?
An obstruction causes pressure to build up within the kidneys. Over time this back pressure can cause damage to the kidneys or cause complications such as kidney failure or infection. It is therefore important to relieve or prevent obstruction of the kidneys.
Temporary relief of the obstruction
It is not always possible to identify and treat the cause of the obstruction, however, it is essential to relieve the obstruction as early as possible to allow investigation or further treatment at a later date once the cause is known. Placing a ureteric stent will form a channel to allow the urine to pass the level of obstruction and allow the kidney to drain better.
What is a ureteric stent?
A ureteric stent is a hollow tube which runs the length of the ureter from the kidney to the bladder. It is made of a flexible plastic material and usually measures between 22 and 26 centimetres.
How does a stent stay in place?
The stent is held in place by a coil at the top within the kidney and a coil at the bottom within the bladder. The stent is flexible and moves with any body movements.
Advantages of having a ureteric stent
- Stop the constant pain from an obstructed kidney.
- Drain infection from the kidney which can be very serious if left untreated.
- Protect the kidney from permanent damage due to prolonged blockage or infection.
- Gently widen the ureter to allow future successful surgery.
How is a ureteric stent put in place?
This is usually placed in the ureter under a general anaesthetic (while you are asleep). A telescope (cystoscope) is passed through the urethra into the bladder. The stent is placed over a wire into the ureter and kidney via the opening of the ureter in the bladder. The stent may also be inserted as an additional part of an operation on the ureter and kidney (ureteroscopy). Occasionally it may be inserted via the kidney, under local anaesthetic, using special X-ray techniques.
The stent is checked to be in the correct position by taking an X-ray at the end of the procedure or occasionally after the procedure.
How long will the stent stay in the body?
The stent is usually kept in place until the obstruction is relieved and will depend on the cause of the obstruction and its treatment. Most stents can stay in place for up to 12 months, however if used for stone disease, we prefer to limit this time to 3 months maximum.
There are some special metallic stents which may be left in for a much longer time. These are used less frequently and will be discussed with you in advance if you are considered suitable. Your urologist will tell you how long they expect your stent to remain in place.
How is a stent removed?
This will depend on whether a string has been left on the outside or not. We leave the string if the stent is only to be in position for up to 2 weeks.
If the string is present then removal is straightforward. You will be asked to attend an appointment with one of our specialist nurses who will ask you to lie down. The stent will then be removed by pulling the string. It is important that you do not cut this string if it is left in place.
If the stent is due to stay in place for longer than 2 weeks then the string will be removed after the stent is placed. You will then require a flexible cystoscopy to allow us to look into your bladder. We will pass graspers via the cystoscope to allow us to hold on to the lower end of the stent and remove it. This procedure only takes 5 minutes or so and is performed under local anaesthetic.
Is there an alternative option?
The only alternative option would be to have a tube inserted directly into the kidney which will drain the urine to the outside. This is called a nephrostomy tube. In some cases, this will then allow us to place a stent from the kidney down to the bladder. However, some patients may have to have a urine collection bag attached to collect the urine drained on the outside. This will need care to prevent it coming out and will require the district or practice nurse involvement.
If you need this treatment your urologist will explain in detail what is involved.
Possible side effects
Ureteric stents are designed to allow people to lead as normal a life as possible. However, they may cause some side effects. These are not normally a danger to your health or your kidney but can affect your quality of life.
Many patients do not experience problems with the stent however, the majority of patient are aware of its presence.
Commonly noted side effects
Urinary symptoms
- Increased frequency of passing urine.
- Urgency - the need to rush to pass urine.
- Blood in the urine. This is quite common, especially after exercise. The situation can improve with an increased fluid intake.
- A sensation of being unable to completely empty the bladder.
- Very occasionally, especially in women, there is a risk of episodes of incontinence, usually due to urgency These side effects improve when the stent is removed.
Discomfort or pain
Stents can cause discomfort or pain, commonly in the bladder and kidney (loin) area, but sometimes in other areas such as the groin, urethra and genitals.
Discomfort or pain may be more noticeable after physical activities and also after passing urine.
It has been reported that around 20 to 70% of patients with stents in place experience one or more of these side effects. In some patients the symptoms of pain while passing urine and blood in the urine may improve with time.
Medical science and the stent manufacturers continue to work to develop a stent that will cause the least possible side effects.
Can the side effects interfere with my day-to-day life?
The majority of patients are able to continue with their normal day to day life, however there are some patients who experience more significant symptoms and may need to adjust their activities.
Physical activities and sports
You can continue with physical activities while the stent is in place provided your health allows you to do so. You may experience some discomfort in the kidney area and passing of blood in your urine, especially if you take part in sports and other strenuous activities
Work activities
You can continue to work normally with the stent inside your body. However, if the work involves a lot of physical activities, you may experience more discomfort. Side effects, such as urinary symptoms and pain associated with the stent, may make you feel tired. If the stent causes significant problems, you should discuss it with your employer as they may be able to make some temporary adjustment to your workload.
Social life and interactions
The stent should not affect your social life greatly but if you experience urinary symptoms such as increased frequency and urgency, you may need to use public toilets more frequently.
Travel and holiday
It is possible to travel with a stent in place, provided the underlying kidney condition and your general health allows this. However, side effects associated with the stent may make travel and holidays less enjoyable. There is a small possibility that you may require additional medical help while the stent is in place so you should inform your insurance company prior to travelling.
Sex
There are no restrictions on your sex life due to the presence of a stent. Some patients experience discomfort during sexual activities and occasionally the side effects associated with having the stent may have an effect on your sexual desire.
If you have a stent with a thread coming out through the urethra, sexual activities may be more difficult and there is the risk of displacement of the stent. We would recommend you avoid intercourse until the string and stent has been removed.
What other complications are possible?
Occasionally a stent may develop a crystal coating on its surface, similar to kidney stones. This is not usually a problem unless the stent has been in place for a long period of time.
Very occasionally a stent may get displaced, usually slipping towards the bladder, it may even fall out. If this happens, you should contact the hospital using the contact details at the end of this page or your GP.
Is there a possibility of a urinary tract infection?
Having a stent in place and an underlying kidney problem makes it more likely that you could get a urinary tract infection. Symptoms of a urinary tract infection include a raised temperature, increased pain or discomfort in the kidney or bladder area, a burning sensation while passing urine and feeling unwell. Please contact your GP for advice as treatment with antibiotics may be needed.
Often the side effects related to the stent are mistaken for infection and so it is important that the urine is tested to assess for infection.
Self-care
- You must drink at least 2 litres (about 4 pints) of fluids, mainly water, each day. We would recommend 15mls of lemon juice in a glass of water with meals to avoid stomach irritation. This will help to cut down the risk of getting an infection and reduce the amount of blood in the urine. Adding lemon juice to water can help prevent stone formation on the stent.
- If you experience bothersome pain, please ask your GP or pharmacist for advice about pain relief. We would recommend tamsulosin 400mcg once a day for pain and solifenacin 5-10mg once a day, for bladder irritation.
- If you have a stent with a thread coming down from the urethra outside the body, then you will need to be careful not to dislodge the thread. If you have any concerns, please contact the Urology Department using the details at the end of this page.
When should I call for help?
You should contact your GP or the Urology Department using the details at the end of this page:
- If you experience a constant and unbearable pain associated with the stent.
- If you have symptoms of a urinary tract infection as mentioned above (a raised temperature, pain during passing urine and feeling unwell).
- The stent gets dislodged, falls out or you develop new incontinence (leakage of urinary).
- If you notice a significant change in the amount of blood in your urine.
Contact information
If you have questions or problems following your stent placement, help or advice can be obtained from:
Urology
Tivoli Ward
Cheltenham General Hospital
Tel: 0300 422 3571 or
Tel: 0300 422 3844
Urology Advanced Nurse Practitioners
Urology Department on Oakley Ward
Cheltenham General Hospital
Tel: 0300 422 5193
Monday to Friday, 8:00am to 4:00pm
Your Consultant’s Secretary
Tel: 0300 422 2222 (when prompted ask for your consultants’ secretary)
Monday to Friday, 8:00am to 4:00pm
Further information
The British Association of Urological Surgeons (BAUS) patient leaflets
Website: https://www.baus.org.uk/default.aspx
My Stent Details
Your healthcare professionals will provide you with details such as; your consultant name and contact, Stent indication, the date of insertion, and any planned duration/future plan.