How to look after your dialysis access
This page gives you the information you need to help you care for your AV Fistula or AV Graft after you have been discharged from hospital.
Your wound will be closed by:
- Stitches that dissolve
- Steri-strips to the skin
- Stitches that need to be taken out
Your wound will be closed with either Stitches that dissolve, Steri-strips to the skin or Stitches that need to be taken out.
If you have stitches that need to be taken out after you go home, an appointment will be made with the access nurse at Gloucestershire Royal Hospital who will take them out and check your wound; if you are having dialysis, staff at your renal unit will change your dressings and take out any stitches. Your team will advise the next steps.
Looking after your wound
Your nurse will check your wound dressing before you are discharged from hospital. If you stay in overnight, your dressing may be changed before you go home if there has been any leakage.
You will be given a spare dressing to take home, and shown how to put it on, in case the one you have over your wound peels off.
We advise you to keep the wound dry and covered for the first 4 days. It is best if the dressing from theatre is left undisturbed for the first 4 days after your operation. Try to keep the wound covered until the stiches or staples have been taken out.
If there is some bleeding through the dressing during the first 24 hours after surgery, a pad of sterile gauze should be stuck on top of the dressing you are wearing.
If there is a lot of bleeding, please contact the hospital (where you were treated) for advice. The contact numbers are at the end of this page.
Infection
Signs of infection in the wound may be:
- Redness and swelling around the wound area
- A cloudy coloured leakage (discharge) from the wound
- A smelly leakage from the wound
- You feel generally unwell
- Increased pain in and around the wound area Contact the Renal Unit as soon as possible if you think you may have an infection, as you could need antibiotic treatment.
Pain
You may have some pain or discomfort from the wound area for a few days. Paracetamol is safe to take in renal failure as long as you follow the instructions on the packet.
If you are allergic to paracetamol, or have been advised not to take it, please find out which pain relief is safe for you to take from your doctor before being discharged. Your GP would also be able to advise you on pain relief medication.
Bruising
It is normal to have some bruising for up to 2 weeks after the operation.
Circulation problems
Your hand or fingers of the arm with the fistula can feel cool, this is quite normal. The coolness is due to the fistula diverting arterial blood away from the hand and into the vein. Sometimes too much blood is moved away from the hand, so if your hand becomes very cold or numb, it is important that you contact Ward 7b or the renal specialist nurse for advice.
Unusual sensation
Some patients find they have unusual sensations, such as numbness or tingling, often over the thumb if the fistula is at the wrist. This usually wears off after a couple of weeks, although it can last longer in some patients. If you are worried, contact your GP, Ward 7b or the renal specialist nurse for advice.
Swelling
Your arm and hand may become swollen after the operation, especially following a graft.
A graft is a biosynthetic tube which is used when it is not possible to create an AV Fistula from a vein and artery. It is possible to use this type of access 2 weeks after surgery.
If your arm is swollen after the surgery, we advise you to rest your arm on a cushion or pillow when sitting down. If you raise your hand to shoulder height some of the time it may reduce some of the swelling. Try to wiggle your fingers from time to time to reduce swelling and prevent stiffness. If the swelling becomes worse and you are worried, contact Ward 7b or the renal specialist nurse for advice.
Bleeding
Blood loss from a fistula or graft can usually be controlled by applying pressure to the site. Avoid using large absorbent dressings and/or towels as this will reduce the pressure applied and its effectiveness to control the bleeding.
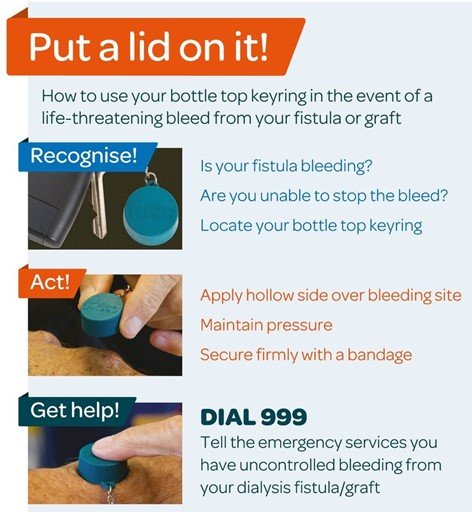
If a bleed from your fistula or graft cannot be stopped with direct pressure over the affected area, locate your bottle top and apply with the hollow side facing your skin, maintaining pressure.
By applying the bottle top to the bleed in this way you will have sealed the bleeding area. This will encourage the blood to clot more quickly.
If no blood is seen coming out from underneath the bottle top, it is safe to assume that the bleeding is controlled. If possible, secure the bottle top firmly with a bandage.
You must then contact Ward 7b or NHS 111 informing them that you have uncontrolled bleeding from your dialysis fistula or graft.
How will I know if my fistula is working?
A successful fistula has a fast flow of blood from the artery into the vein. This can be heard through a stethoscope as a ‘whooshing’ noise or felt as a ‘buzzing’ sensation. The nurse will check your fistula after the operation to see if it is working. You will be shown how to do this.
When your fistula is new, check it at least twice daily. After a few weeks it should be checked at least once a day. It can take 3 months or more until the fistula is ready to use for dialysis treatment.
If you cannot hear or feel the blood flow, or it seems weaker, please contact Ward 7b or your specialist nurse for advice.
Care of your fistula or graft
- Keep your fistula or graft limb warm
- Do not let anyone take blood, put in a drip, insert a needle or take your blood pressure on your fistula or graft arm
- Do not wear tight clothing, a wristwatch or tight jewellery on your limb as this could limit the blood flow and damage your fistula or graft
- Do not pick scabs on your access arm or leg as this could cause infection
- Do not have a tattoo on your access arm or leg
- Try not to sleep on your access arm
Follow up
- You will be given a follow up appointment at Gloucestershire Royal Hospital with a renal nurse to assess the wound. The appointment will be made for 5 to 7 days following your operation.
- The renal team will check the progress of your fistula over the next 8 to 12 weeks. If you are having dialysis already, your dialysis nurse will also check the progress of your fistula and will tell you when it is ready to use.
- If you are not yet on dialysis, you will be reviewed by the surgeon 6 to 8 weeks after your operation. Arrangements will be made for you to be seen as an outpatient at the hospital.
Exercises to help your fistula to develop
Over the next 6 to 12 weeks the fistula vein needs to stretch in diameter (width) so that it is large enough to take dialysis needles. During the dialysis treatment the dialysis machine will take out and put back large volumes of fluid. For this to be successful the fistula vein needs to develop a strong thrill or buzzing sensation, sometimes exercising the arm can help.
If you have a fistula, there are some simple exercises you can do that may help it develop. The renal specialist or dialysis nurse will explain these to you and tell you when you should start them. This is usually when the operation wound has fully healed, normally after 2 weeks.
The exercises are simple and can be done sitting down.
- Hold a soft ball, a sponge or a rolled up pair of socks in your hand. Squeeze the object 10 times then relax. Repeat this 4 or 5 times every day, if you can.
This exercise should not be tiring, but if you have any concerns, please consult a doctor or nurse before starting them.
If you have a graft, there is no need to do these exercises.
Contact information
If you any questions or concerns and you are already on dialysis, please contact the haemodialysis unit you are attending:
Cotswold Renal Haemodialysis Unit
Tel: 0300 422 6848
Tel: 0300 422 6639
Monday to Saturday, 7:00am to 11:00pm
Severn Renal Satellite Unit
Tel: 0300 422 6077
Monday to Saturday, 7:00am to 11:00pm
Forest Renal Satellite Unit
Tel: 0300 422 8762
Monday, Wednesday and Friday, 7:00am to 7:00pm
If you are not yet on dialysis please contact:
Ward 7b
Gloucestershire Royal Hospital
Tel: 0300 422 6768 (open 24 hours a day)
If you need to contact Cheltenham General Hospital:
Tel: 0300 422 2222
When prompted, ask for the ward you were discharged from (open 24 hours a day)
If you require further information, please contact:
Renal Access Nurse
Gloucestershire Royal Hospital
Tel: 0300 422 6270
Monday to Friday, 8:00 to 3:00pm
Teaching and training
Gloucestershire Hospitals NHS Foundation Trust is involved in the teaching or training of medical staff who may be in attendance at some patient consultations. However, there is an 'opt out' option for any patient who would rather see a doctor without training medical staff in attendance.