Care of your cast
This page gives you information about looking after your plaster cast. Taking good care of your cast will help with your recovery.
On this page
-
About your cast
-
Care of your limb and cast
-
Do not get your cast wet or near heat
-
Do not cut your cast:
-
Reducing the risk of a blood clot when in a plaster cast
-
Who is at risk of a VTE?
-
Reducing the risk of developing VTE
-
Signs and symptoms of DVT and PE
-
Washing and dressing
-
Sleeping
-
Eating and drinking
-
Exercises for when your arm is in a cast
-
Exercises for when your leg is in a cast
-
Sport
-
Can I drive?
-
Can I go on holiday?
-
Future appointments
-
Contact information
-
Further information
About your cast
If your cast is ‘Plaster of Paris’ it will feel warm for 20 minutes and take about 48 hours to dry.
Synthetic casts will feel warm for about 3 minutes and will take about 30 minutes to dry.
Care of your limb and cast
While you are in a cast, keeping your limb raised will help relieve any pain you may be feeling.
Please be aware that the cast will not relieve all of your pain. We recommend that you take regular pain relief for the first few weeks of your injury if needed.
If you are using a sling, remember to move your elbow and shoulder as advised.
Skin damage under the cast
Sometimes your cast can rub your skin and can cause a blister to form under the cast. This needs to be treated as soon as possible to stop it from getting worse. Please contact the Plaster Room for advice as soon as possible. the telephone number is at the end of this page.
If you have an increase in pain, an unusual odour from the cast, any rubbing, burning or any other concerns, you should contact the Paster Room for advice as soon as possible. The staff will give you an appointment time to attend and ask that you report to the Trauma & Orthopaedic reception on your arrival.
Damage to your cast
If your plaster cracks, becomes loose or if you have dropped something inside your cast, please contact the Plaster Room.
Swelling and pain
Keep your arm or leg raised on a soft surface, such as a pillow, as often as possible while your limb is in plaster. This will help any swelling to go down and will reduce the feeling of pins and needles in your limb.
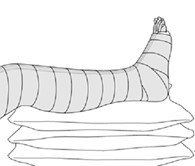
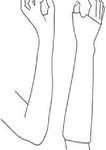
Reduced circulation
If your fingers or toes become cold and blue, even if you have kept your limb raised, please contact the Plaster Room immediately for advice.
Do not get your cast wet or near heat
Do not cut your cast:
Reducing the risk of a blood clot when in a plaster cast
Having a plaster cast can make you less active and increase the risk of blood clots (venous thromboembolism – VTE).
VTE is the collective name for deep vein thrombosis (DVT) and pulmonary embolism (PE). VTE can be a serious and life-threatening condition.
DVT is the name given to a blood clot which forms inside a vein, deep beneath the skin of your leg. The clot blocks the blood flow through the affected vein and can cause several signs and symptoms.
Sometimes, a part of the clot breaks off and passes through your veins which can block a blood vessel in your lung - this is called a PE.
Who is at risk of a VTE?
Some people are more at risk than others of developing a blood clot. The risk is increased if you:
- are over 60 years old
- have a personal or family history of blood clots
- have active cancer
- have recently had major surgery
- have an Achilles tendon rupture
- have had a baby in the last 6 weeks or you are currently pregnant
- have a disorder which makes your blood more likely to clot
- take certain medications, such as the combined oral contraceptive or hormone replacement therapy
- have long-term medical conditions requiring treatment, such as heart, lung, bowel or hormone disease
- are overweight
- have varicose veins
Reducing the risk of developing VTE
A doctor or nurse will complete a simple assessment with you, to work out your personal risk. If you are considered to be at risk of VTE, your doctor will discuss this with you and may prescribe you a blood thinning medicine called heparin. This is a small injection.
You or your carer will be shown, by a registered nurse, how to injection the heparin into your tummy or outer thigh. The doctor will decide how long the heparin will need to be given.
Whether you have been prescribed heparin or not, you should take the following precautions:
- Try to keep moving around as much as possible (unless you have been advised otherwise)
- Drink plenty of fluids to avoid becoming dehydrated
- Take pain relief regularly as needed. Follow the dosage instructions inside the package
Signs and symptoms of DVT and PE
DVT
- Leg pain or tenderness
- Leg swelling
- Leg is warm to touch
- Redness of leg
PE
- Shortness of breath or difficulty breathing
- Chest pain
- Coughing up blood
- Sudden collapse
However, a DVT or a PE may happen without any symptoms.
If you develop any of the signs and symptoms above, you should contact your GP or NHS 111 immediately for advice.
If you have severe shortness of breath, chest pain or you collapse, you or the person with you should dial 999 for an ambulance.
Washing and dressing
We advise you to use waterproof protection when you have a bath or shower. There are many types and brands available online and from your local pharmacy.
We do not suggest the use of plastic bags as they can leak.
Many patients find it easier to have a strip wash while in plaster.
Dressing may be difficult. It is usually easier to wear clothes which are loose fitting. When dressing we recommend that you put the injured limb into the clothing first and take it out last when getting undressed.
Sleeping
You may find it difficult to sleep at first but most people find that after a few nights it is more comfortable. Resting your cast on a pillow may help you get a better night’s sleep.
Eating and drinking
You are advised to eat a well-balanced diet which is rich in protein to help with the bone development and repair. This includes meat, fish, eggs, cheese (or vegetarian alternatives), milk, nuts and pulses.
Exercises for when your arm is in a cast
These exercises are important, as they will prevent joint stiffness and poor circulation. Repeat these exercises 5 times every hour during the day.
1. Shoulder movement
Standing or sitting in an upright position, slowly lift your affected arm up towards the ceiling (elbow straight) and then lower again. Repeat 5 times.
2. Elbow moving and stretching
Sitting in an upright position, slowly bend your affected elbow so your hand moves towards your shoulder and then fully straighten your elbow. Repeat 5 times.
3. Finger exercises
Place the elbow of your affected arm on the table with your fingers pointing towards the ceiling (as shown below).
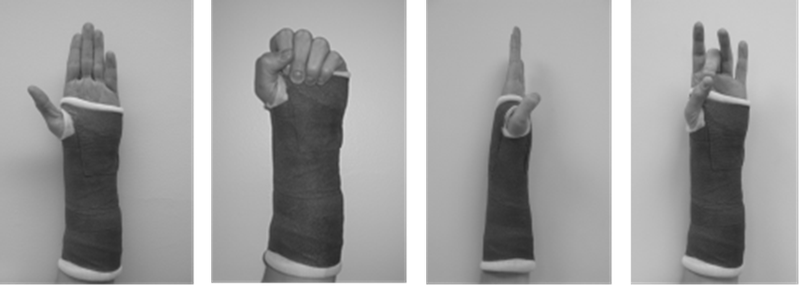
Start with all your fingers straight:
- Bend all your fingers to make a fist
- Bend your hand at the large knuckle joints while trying to keep your fingers straight
- Bend your finger joints to form a ‘hook’ position, hold for 2 to 3 seconds then release
- Touch the tip of each finger with your thumb
- Move your thumb towards the base of your little finger and then fully straighten the thumb. These exercises can also be carried out if your cast includes your elbow.
Exercises for when your leg is in a cast
Toe exercises
Wiggle your toes whenever you remember. Curl your toes under, hold for 5 seconds and release. Stretch your toes out, hold for 5 seconds and release.
Leg lifts
These help to strengthen the muscles in your ankle and leg while wearing a cast. Lie on the floor, keeping your leg and knee straight. Raise your leg several inches above the floor and hold for 5 seconds. Bring your leg back down to the floor.
If your knee is not in a cast, include bending and straightening the knee while sitting in a chair.
Repeat these leg and toe exercises 10 times each day.
Sport
You are advised not to take part in contact sports such as football or rugby.
Do not attempt swimming or any other water sports.
Can I drive?
You must check with your insurance company before driving. Your insurance may be invalid which can lead to you being liable to prosecution.
Can I go on holiday?
If you are going on holiday, sea and sand must be avoided while you have your plaster cast.
Please discuss with your GP or travel provider if you are traveling by air.
When travelling to Europe, do not forget your ‘GHIC’ (UK Global Health Insurance Card), available from www.nhs.uk/using-the-nhs/healthcare-abroad/apply-fora-free-uk-global-health-insurance-card-ghic. Please visit the website for more information.
If your airline requests a letter from the doctor, please mention this to us at your next appointment.
Future appointments
If you are unable to attend your next appointment, please contact the Orthopaedic Outpatients on the number at the end of this page.
If you are expecting to receive an appointment either by phone or letter and you do not hear from us within 48 hours of your cast being applied then please contact the Trauma Service on the number at the end of this page.
Remember to take pain relief before attending any appointments as we may be removing or changing the plaster cast.
Contact information
Trauma Service enquiries
Tel: 0300 422 5269
Monday to Friday, 8:00am to 2:00pm
Plaster Room
Cheltenham General Hospital
Tel: 0300 422 3148
Monday to Friday, 8:30am to 4:30pm
Gloucestershire Royal Hospital
Tel: 0300 422 8411
Monday to Friday, 8:30am to 4:30pm
Outside of these hours you can contact NHS 111 for advice. Tel: 111
Further information
Crutches, walking frames and raised toilet seats should be returned to:
Telephone: 0300 421 8100

