Having a colonoscopy as an inpatient
You have been advised to have a colonoscopy to help investigate the cause of your symptoms. It is important that you read this page before your appointment so that you understand what will happen during the procedure and the preparation involved.
What is a colonoscopy?
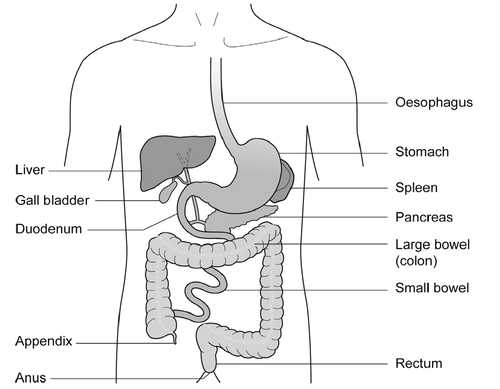
Colonoscopy is an investigation to look directly at the lining of the large bowel (colon). In order to do this, a colonoscope is passed through the anus (back passage) and into the bowel.
A colonoscope is a long flexible tube, about the thickness of your index finger; with a bright light at the end (this is not hot). By looking at the screen the doctor can see the lining of the bowel and check whether any disease is present.
The colonoscopy will also allow for some treatments to be performed.
Biopsy
A biopsy is a small sample of tissue that may be taken from the lining of your gut or bowel for further examination in the laboratory. It is taken using sterile biopsy forceps through the scope. This will not be painful.
Polyps
It is possible to remove polyps during a colonoscopy using a special snare. Polyps are abnormal bits of tissue, like warts, which the doctor will want to examine in more detail. This procedure is not painful.
There are other therapeutic procedures which can be done during a colonoscopy such as stretching of the bowel when there is a narrowing and argon therapy for the treatment of areas that are bleeding.
Preparation for your procedure
The test and possible complications will have already been explained to you so that you understand the procedure and any risks involved.
You will be asked to sign a consent form by the ward doctor. By signing this form, you will have agreed to have the test performed and that you understand why it is needed. This does not take away your right to have the test stopped at any time.
To allow a clear view during the procedure the bowel must be cleaned using a special oral (taken by mouth) preparation. Your doctor will prescribe a bowel preparation. It is important that you drink all of the preparation before your procedure goes ahead as this will give the endoscopist the clearest views of your bowel.
You will not be able to eat anything while you are preparing for your colonoscopy but you can drink clear fluids while taking the preparation right up to your appointment time.
Clear fluids can be black tea or coffee, Bovril® or Oxo®, any squash except blackcurrant as it stains the bowel, clear apple juice or any other clear juice as long as it does not contain bits.
On arrival at the Endoscopy Unit
You will be seen by a nurse who will check your paperwork and record your observations.
A nurse will then take you into the room where your colonoscopy will take place. Depending on how you have travelled to the Endoscopy Unit, you will either be on your hospital bed or one of the Endoscopy trolleys. You will be made comfortable on your left side with your knees bent. A nurse will stay with you throughout the test.
A rectal examination may be done as part of the procedure. This is where a doctor uses their finger to check for any problems inside your bottom(rectum). It is usually very quick and you should not feel any pain. Sometimes a nurse will assist the endoscopist by applying some pressure to your abdomen (tummy) with their hand. This can often help the endoscope to progress through your bowel more efficiently.
A colonoscopy normally takes 20 to 40 minutes.
Intravenous sedation
Sedation will be given into a vein in your hand or arm. This will make you lightly drowsy and relaxed but not unconscious. You will be in a state called conscious sedation. This means that, although drowsy, you will still hear what is said to you and therefore will be able to follow simple instructions during the investigation. Sedation also makes it unlikely that you will remember anything about the procedure.
You will be able to breathe normally during the procedure.
If suitable, Entonox® (gas and air) is also available during the procedure either as an alternative to sedation or as well as sedation. This will help to control any discomfort.
If you have experienced any of the following within the last 12 weeks, Entonox® will not be suitable for you.
- Pneumothorax
- Air embolism
- Bowel obstruction
- Head injury that has required an overnight stay in hospital
- Decompression sickness
Entonox will also not if suitable if:
- You have emphysema/COPD
- You have had recent ear/eye surgery
- You have been scuba diving in the last 12 weeks
Possible complications associated with having sedation
Sedation can sometimes cause problems with breathing, heart rate and blood pressure. If any of these problems happen, they are normally short lived.
Careful monitoring by a fully trained endoscopy nurse makes sure that any problems are identified and treated rapidly.
Older patients and those who have health problems, for example, people with breathing difficulties due to a respiratory condition will be assessed by a doctor before the procedure.
Benefits of having a colonoscopy
- To diagnose and treat a possible cause of symptoms
- To review results of any previous endoscopy
Possible risks
Complications are uncommon with diagnostic (investigative) procedures and are mostly due to the sedation given. Major complications are very rare.
Serious or frequently occurring risks
- If a biopsy is taken or a polyp removed it can lead to bleeding or a perforation (a tear) of the bowel. This happens in less than 1 in 5,000 cases and rarely blood transfusions and/or surgery is needed. If surgery is needed it will be a major operation but the risks of complications are small.
- Bleeding when a biopsy is taken or removal of polyp is 1 in every 500 cases.
- The overall chance of missing something important such as a cancer is less than 1 in every 2,500 cases.
- Abdominal discomfort mostly around the low left-hand side of the abdomen.
- Adverse reaction to any medication given.