Having a gastroscopy and colonoscopy
You have been advised to have a gastroscopy and colonoscopy (also known as an endoscopy) to help investigate the cause of your symptoms. It is important that you read this information before your appointment so that you understand what will happen during these procedures and the preparation needed.
Medication
If you take medicines containing iron, you must stop taking them 7 days before your appointment.
If you have diabetes and you are receiving treatment, please contact the Medication Advice Line. You will be asked to leave a message; a member of staff will return your call. The number is at the end of this page. If you are an insulin pump patient, we would like your BM to be 7mmol/L. Please contact your local pump team if you need further advice.
If you are taking any medication that thins your blood, other than aspirin (which you can continue to take) or you are pregnant please seek advice from your GP, referring consultant or the Medication Advice Line.
This is very important as your procedure may be delayed if you do not get advice.
What is a gastroscopy?
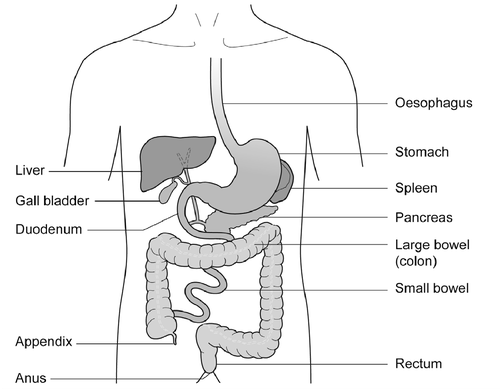
Gastroscopy is an investigation to look directly at the lining of the oesophagus (gullet/food tube), the stomach and around the first bend of the small intestine (the duodenum). A gastroscope is passed through the mouth, down the oesophagus and into the stomach.
A gastroscope is a long flexible tube, thinner than your little finger. It has a bright light at the end (this is not hot), which is necessary to be able to see the lining of the stomach.
Pictures are transmitted onto a screen where any abnormalities can be seen. The gastroscopy will allow for some treatments to be performed.
What is a colonoscopy?
Colonoscopy is an investigation to look directly at the lining of the large bowel (colon).
In order to do this, a colonoscope is passed through the anus (back passage) and into the bowel. A colonoscope is a long flexible tube, about the thickness of your index finger; with a bright light at the end (this is not hot). By looking at the screen the doctor will be able to see the lining of the bowel and check whether any disease is present.
It will be necessary to ask you to roll onto your back or right side during the procedure. This helps the endoscopist to have a clearer view of the lining of the bowel. The colonoscopy will also allow for some treatments (therapeutic procedures) to be performed.
Treatments
Biopsy
A biopsy is a small sample of tissue that may be taken from the lining of your stomach or bowel for further examination in the laboratory. It is taken using sterile biopsy forceps through the colonoscope. This will not be painful.
Dilatation
A dilatation can be performed if a narrowing of the gullet (oesophagus) is found. This means stretching the narrowing to help improve your ability to swallow. Usually, the need for this procedure has been identified before your appointment.
Dilatation is not available in Stroud or Cirencester hospitals.
Banding
Piles (haemorrhoids) can be banded but you will need to be on a surgeon’s list for this to happen.
Removal of polyps
It is possible to remove polyps during a colonoscopy using a special snare. Polyps are abnormal bits of tissue, like warts, which the doctor will want to examine in more detail. This procedure is not painful.
Other therapeutic procedures
There are other therapeutic procedures which can be done during a colonoscopy such as stretching of the bowel when there is a narrowing and argon therapy for the treatment of areas that are bleeding.
Alternative procedures
The main alternative to a gastroscopy is a barium meal X-ray. This can look at the stomach, but does not allow biopsies to be taken.
The main alternative to a colonoscopy is a CT Colonography (scan of the colon). This is performed in the X-ray department. A CT Colonography does not allow any therapeutic therapies to be performed.
Please note that an alternative procedure will not be available on the day of your appointment.
Preparation for your procedure
To allow a clear view during the procedure the bowel must be cleaned using a special preparation.
You should have received your bowel preparation and full instructions on how to take it. This will also include details of what you can eat and drink before the colonoscopy.
If you have not received the preparation, or have any questions about it, please telephone the Medication Advice Line. The telephone number is at the end of this page.
Please note that you can drink clear fluids while taking the preparation right up to 2 hours before your appointment time.
Clear fluids can be black tea or coffee, Bovril® or Oxo®, any squash except blackcurrant as it stains the bowel, apple juice or any other juice as long as it does not contain bits.
The NHS, a major contributor of carbon emissions in the UK, has recently outlined ambitious targets to achieve net zero carbon emissions by 2040. The endoscopy team in Gloucestershire have carefully considered ways of adopting more sustainable care and waste reduction. We would appreciate your support to help make our practice ‘greener’ by kindly bringing the following items along to your endoscopy appointment, so that single use alternatives are not required:
- If applicable, your own denture pot, hearing aid case(s) and/or eyeglasses case
- Water bottle
- Reusable cup with lid for a complimentary hot drink after the procedure
On admission
On arrival at the department, you will be seen by a nurse who will check your personal details.
You will be asked a series of questions about any operations or illness that you may have had or are presently suffering with.
Please bring a list of all medications you are currently taking.
The nurse will also ask if you have any allergies or if you have had any reactions to medicines or foods.
You might also be given a small dose of Parvolex® and Infacol®, by mouth, to reduce the secretions in your oesophagus and bowel. It will also give a better view of your oesophagus and stomach during the procedure. Please do not have any other liquids after you have been given the Parvolex® and Infacol® - the nurse giving you this medication will also remind you not to have any further fluids.
You will be asked if you want sedation. If you are considering sedation, you will be asked to confirm that you have a responsible adult to escort you home when you are ready for discharge. You must also have a responsible adult with you at home for 24 hours following the procedure.
The test and possible complications will be explained so that you understand the procedure and any risks involved.
You will be asked to sign a consent form. By signing this form, you will have agreed to have the test performed and that you understand why it is needed. This does not take away your right to have the test stopped at any time.
For the time that you are in the department we want to provide a safe, supportive and pleasant environment. Please do not be afraid to ask if you have any questions or worries at this stage.
As you are having both gastroscopy and colonoscopy procedures, you will be asked to change into a hospital gown.
Please remember that your appointment time is not the time you will have your procedure. There will be a waiting time between your admission and having your procedure done.
Throat spray or sedation
Local anaesthetic throat spray and/or intravenous sedation can improve your comfort during the procedure. Intravenous sedation will make you lightly drowsy and relaxed, but not unconscious (asleep).
Anaesthetic throat spray
Throat spray is a local anaesthetic spray used to numb the throat. This can be given on its own or alongside sedation.
As the gastroscopes have become thinner, many patients are happy for the procedure to be carried out without sedation and to have throat spray instead.
The throat spray has an effect very much like a dental injection.
The only restriction is that you must not have anything to eat or drink for about an hour after the procedure. This will allow for the sensation in your mouth and throat to return to normal.
It is strongly advised that your first drink after the procedure should be cold. This should be sipped slowly to make sure that you do not choke.
Intravenous sedation
Sedation will be given into a vein in your hand or arm. This will make you feel lightly drowsy and relaxed but not unconscious (asleep). You will be in a state called conscious sedation. This is not the same as a general anaesthetic. Sedation means that, although drowsy, you will still hear what is said to you and therefore will be able to follow simple instructions during the procedure. You will be able to breathe normally throughout the procedure.
While you are sedated, we will check your breathing and heart rate so changes will be noted and dealt with accordingly. For this reason, you will be connected by a finger probe to a pulse oximeter which will measure your oxygen levels and heart rate during the procedure. Your blood pressure will also be recorded. Oxygen will be given to you via a small sponge inserted into your nostril. Please note that if you decide to have sedation you are not allowed to drive, drink alcohol, operate heavy machinery or sign any legally binding documents for 24 hours following the procedure.
You will also need a responsible adult to accompany you home and stay with you for 24 hours.
Entonox®
Sometimes Entonox® (gas and air) may be offered, either as an alternative to sedation or as well as. This will help to control any discomfort. You will not need a responsible adult to stay with you if you choose Entonox® only (a leaflet will be provided).
The procedures
A nurse or doctor will escort you into the room where your procedures will take place. You will be made comfortable on a patient trolley lying on your left side, with your knees slightly bent. A nurse will stay with you throughout the test.
In the examination room, any dentures will be removed and the local anaesthetic spray will be applied to numb the back of your throat.
To protect your teeth and the gastroscope a plastic mouth piece will be put between your teeth (or gums if dentures have been removed). The tube will then be inserted through the mouth piece. When it reaches the back of the throat you may be asked to swallow to help the tube go down into the stomach. This will not interfere with your breathing.
Some air will be passed through the gastroscope to stretch the stomach to allow a clearer view. You may feel wind like discomfort and belch up some air during the test. Please do not be embarrassed.
Any saliva in your mouth will be removed using a small suction tube. When the gastroscope is taken out most of the remaining air in the stomach will also be removed. The gastroscopy normally takes about 5 minutes.
Once the gastroscopy is complete the equipment will be changed for your colonoscopy procedure. The trolley will be moved to make sure that you are in the correct position for the colonoscopy.
A rectal examination may be done as part of the procedure. This is where a doctor uses their finger to check for any problems inside your bottom (rectum). It is usually very quick and you should not feel any pain.
During this procedure you will experience some abdominal bloating and discomfort due to the air that will be introduced through the scope into the large bowel. Sometimes a nurse will assist the endoscopist by applying some pressure to your abdomen (tummy) with their hand. This can often help the endoscope to progress through your bowel more efficiently.
The colonoscopy will take about 20 to 40 minutes.
Possible complications
Sedation can occasionally cause problems with breathing, heart rate and blood pressure. If any of these problems occur, they are normally short lived.
Careful monitoring by a fully trained endoscopy nurse makes sure that any potential problems can be identified and treated rapidly. Older patients and those who have health problems, for example people with breathing difficulties due to a bad chest may be assessed by a doctor before being treated.
Minor complications with sedation happen in less than 1 in every 200 examinations. A few people are excessively sensitive to the sedation we use and become too sleepy. This effect can be rapidly reversed with another injection.
Major complications with endoscopic procedures are very rare (less than 3 in 10,000) and death arising from these is extremely rare (less than 1 in 30,000 cases).
The main serious complication is perforation (a tear) of the oesophagus (gullet) or bowel, which may need an operation and stay in hospital.
There is a small risk of bleeding if a polyp is removed at the time of your colonoscopy (less than 1 in 100). The endoscopist will usually be able to stop the bleeding during the procedure.
After the test
After both procedures are completed, the nurse caring for you during your test will take you to the recovery area.
Your pulse and blood pressure will be monitored as needed. This is called the recovery period. You may feel a little bloated or have some discomfort in your lower abdomen after the tests.
You will need to stay in hospital for about 1 hour after the procedures, depending on how you recover from the sedation, if given.
Normally you do not see the person who performed your procedure before going home. Your nurse will tell you the results of the test before you are discharged. If you have had sedation, it is a good idea to have someone with you at this discussion as many people find they forget what has been said to them.
If a sample (biopsy) has been taken, the result can take up to 5 weeks to process. You may be given an outpatient’s appointment to return for review.
Alternatively, the results will be forwarded to your GP; you will need to make an appointment to discuss the results.
A report of the procedure will automatically be sent to your GP.
Going home
If you have had sedation, it is essential that someone takes you home and that there is a responsible adult to stay with you for 24 hours.
Important note: You may go home by taxi but you must have someone to accompany you on the journey. For this period of time, you should not:
- Drive a car, motorbike or ride a bicycle
- Drink alcohol
- Operate machinery or do anything requiring skill or judgement
- Make important decisions or sign any documents If sedation has not been given the above paragraph does not apply.
An advice booklet including this information will be given to you before you leave the department.
Gloucestershire Hospitals NHS Foundation Trust Endoscopy units are training centres. Registrars and Nurse Endoscopists regularly attend endoscopy procedure lists. Please let the admitting nurse know if you have any concerns about this.
Contact information
Appointment Enquiries
Tel: 0300 422 6350
Monday to Sunday, 8:00am to 4:00pm
Medication Advice Line (answer machine)
If you have any questions relating to your medication, please leave a message. A member of staff will return your call normally within 24 hours, Monday to Friday only, excluding Bank Holidays.
Cheltenham General Hospital
Tel: 0300 422 3370
Monday to Friday, 8:00am to 4:00pm
Gloucestershire Royal Hospital
Tel: 0300 422 8232
Monday to Friday, 8:00am to 6:00pm
Saturday and Sunday, 9:00am to12:00 midday
Other Endoscopy Units
Cirencester Hospital
Tel: 0300 421 6294
Monday to Friday, 8:00am to 6:00pm
Stroud General Hospital
Tel: 0300 421 8073
Monday to Friday, 8:00am to 6:00pm