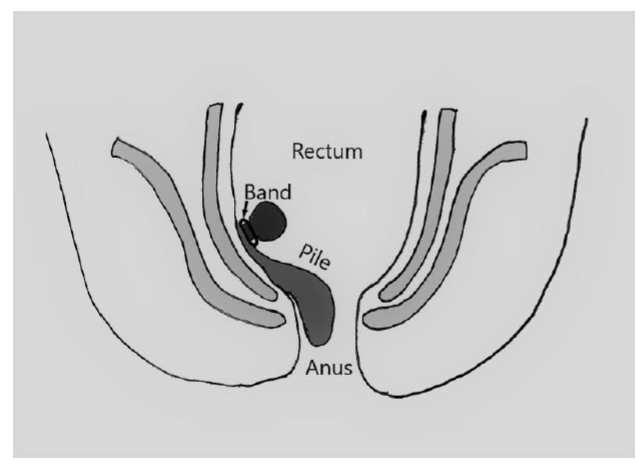
Banding of piles
This page gives you information about the banding of your piles, what to expect after the procedure and the possible complications. It also gives you information about how to stop the piles returning.
What are piles (haemorrhoids)?
The back passage (anus) is normally lined with 3 areas of soft fleshy tissue (cushions) which are very well supplied with blood vessels. In some cases, often because of problems with passing motions, these cushions enlarge over time, forming what we call piles (haemorrhoids). Because of the good blood supply, these piles can cause bright red bleeding usually during or after having your bowels open. They may also prolapse (push out of the anus) or cause mucus leakage and skin irritation.
How does the treatment work?
Banding of piles is done as an outpatient treatment and only takes a few minutes.
Using a short telescope, tiny rubber bands are placed inside the back passage above the piles. This constricts (tightens) and cuts off the blood supply to the piles. Over the next few weeks, the piles then shrivel up, hopefully leading to an improvement in your symptoms.
What to expect after the procedure
Immediately after the banding there may be a sensation of needing to have your bowels open. This is normal – do not worry. The sensation will fade to a mild discomfort or ache lasting a couple of days.
You may feel a little light headed shortly after the procedure. In case you feel faint, it is advisable to sit quietly to let things settle down for 20 to 30 minutes before driving or catching public transport.
Over the next few days, you can take mild pain relief, such as paracetamol, to help with any discomfort.
After 7 to 10 days the tissue in the band will fall away. You may get some dark red bleeding from the back passage at this stage. This is normal – do not worry.
Possible complications of the treatment
Occasionally, bands constrict a part of the lining of the back passage which is very sensitive. This usually gives severe pain at the time the bands are put on. If this happens, the bands may need to be removed.
Very rarely you may get large amounts of bright red bleeding after 7 to 10 days. If this happens you will need to be seen by your GP or at the Emergency Department. This can be more common if you take any medications to thin your blood such as Clopidogrel, Warfarin or Rivaroxaban. If you are currently taking any of these medications your surgeon may recommend that you stop before having the banding carried out.
Banding is a simple and effective treatment for piles but sometimes you may still have remaining symptoms that need repeat banding or alternatively, a different procedure.
When to go to your GP
There is no need to be seen routinely after banding treatment. If you have severe pain in the back passage or persisting or heavy bleeding, you should see your GP for a check-up.
Often your surgeon will leave you with an ‘open appointment’ so that if you have ongoing symptoms (within 6 months of treatment) you can contact their secretary to book an appointment to be seen again in clinic, without having to go back through your GP.
How to stop the haemorrhoids returning
A good bowel habit is the key to stopping haemorrhoids from forming.
- Stop the motions from being too hard. You can help to keep the motions soft by eating a diet high in fibre and drinking plenty of fluids with meals. If necessary, taking mild laxatives which act as stool-softeners such as Laxido® or Fybogel® are available buy at your local chemist.
- Try not to strain when passing motions. Different people have a different number of bowel actions in a day/week. Do not try and strain to have a bowel action unless you feel the need to go and do not try too hard to ‘push out every last little bit’. Some people find it helpful to raise their feet on a step/box to reduce straining.
- Do not spend too long on the toilet. When sitting down, the weight of the body pushes down into the pelvis causing the lining of the back passage to swell. Aim to spend around 5 minutes having a bowel action. Do not take any longer than necessary.